
According to the National Practitioner Data Bank (NPDB), more nurses are called defendants in malpractice lawsuits.
The number of malpractice payments carried out by nurses grew from 253 to 413 between 1998 and 2001.
It doesn’t show any signs of stopping despite the efforts of nursing educators to inform student nurses and practicing nurses of their professional and legal limitations and responsibilities.
Nurses can be charged with negligence due to any failure to act or action that causes patient injury and can lead to a malpractice lawsuit.
Often, it happens due to unintentional failure to follow the standards of clinical practice.
In this article, you will find the analysis of the cases decided from 1995 to 2001 as well as what actions and issues led to charges of negligence that resulted in malpractice lawsuits against nurses.
You will also find out which nursing practice areas appeared in the complaints most frequently.
This article doesn’t include criminal cases based on intentional acts for which nurses were arrested and sometimes prosecuted.
Table of Contents
Defining and Tracking Malpractice
Negligence is defined by the Joint Commission on Accreditation of Healthcare Organizations (JCAHO) as a “failure to use such care as a reasonably prudent and careful person would use under similar circumstances.”
Malpractice is defined by JCAHO as “improper or unethical conduct or unreasonable lack of skill by a holder of a professional or official position; often applied to physicians, dentists, lawyers, and public officers to denote negligent or unskillful performance of duties when professional skills are obligatory.
Malpractice is a cause of action for which damages are allowed.”

There are various definitions of malpractice under institutional policies, state nurse practice standards, or federal guidelines such as JCAHO.
All of them may be considered in court.
The increased number of malpractice cases against nurses is a result of several factors.
Delegation
Due to cost-containment efforts in HMO and hospitals, nurses delegate some of their duties to assistive personnel without proper licensure.
According to the standards of care in a facility or the nurse practice act of the state, this can be considered negligence.
Early Discharge
Patients are discharged with conditions that require more intensive and acute care or at the early stages of recovery.
Nurses can be sued for not making the appropriate referrals to the patient’s condition or for not providing care.
The Nursing Shortage and Hospital Downsizing
Because of this, the workload for nurses has increased, therefore, increasing the likelihood of a mistake.
Advances in Technology
Nurses need to be knowledgeable about the limitations, capabilities, and safety features of technologies.
Increased Autonomy and Responsibility of Hospital Nurses
Nurses exercise advanced nursing skills with more autonomy, which can lead to greater liability and risk of error.
Better-informed Consumers
Being better informed, consumers may know about malpractice issues and be able to recognize inappropriate or insufficient care.
Expanded Legal Definitions of Liability
With this, all professionals are accountable to high standards.
For example, while advanced practice nurses have an expanded scope of practice, they may be held to a medical standard of care by courts.
In 1990, the NPDB started gathering information about the practitioners in health care who had disciplinary action taken against them due to the judgment in malpractice suits.
That resulted in revoked licenses or limited practice.
Some had to pay monetary awards (or their employers or insurance carriers would).
The NPDB was established in 1986 by the Health Resources and Services Administration, Bureau of Health Professions, and U.S. Department of Health and Human Services.
It assists such agencies as hospitals, licensing boards, or HMO in checking practitioners’ qualifications which agencies are looking to hire, grant memberships, licenses, or clinical privileges.
RNs are classified by the NPDB into four categories:
- Nurse-midwives.
- Nurse anesthetists.
- Nurse practitioners.
- Nonspecialized RNs.
RNs have carried out 3,615 malpractice payments over the history of NPDB, according to the data bank.
This includes only the cases reported to the NPDB September 1, 1990, through December 31, 2001.
The most malpractice payments were made by nonspecialized RNs (2,311 or 63.9%).
Next, there were nurse anesthetists with 820 or 22.7% and nurse midwives with 296 or 8.2%.
The fewest number of malpractice payments was made by nurse practitioners of 188 or 5.2%.
The alleged cases of nursing negligence continue to include acts of commission or omission commonly alleged by plaintiffs 20 years ago.

According to annual reports of NPDB, the following nursing negligence issues led to the majority of payments in malpractice suits from 1990 to 2001:
Among nonspecialized RNs:
- Problems related to –
- Monitoring.
- Treatment.
- Obstetrics.
- Medication.
- Surgery.
Among nurse anesthetists:
- Problems related to anesthesia.
Among nurse-midwives:
- Problems related to obstetrics.
Among nurse practitioners:
- Problems related to diagnosis and treatment.
The following nursing negligence issues were identified as the bases of verdicts or settlements in favor of plaintiffs (in the 1997 study):
- Inadequate patient assessment.
- Inadequate infection control.
- Failure to communicate adequate information to the physician.
- Medication errors.
- Nursing interventions.
- Unsafe or improper use of equipment.
- Nursing care.
Noteworthy, claims or payments made in a malpractice action shouldn’t be considered to be a presumption of the guild of a provider.
According to the NPDB, “settlement of a medical malpractice claim may occur for reasons that do not necessarily reflect negatively on the professional competence or conduct”.
For instance, the insurance carrier of a provider could settle without the consent of a policyholder, under the terms of the nurse’s insurance policy.
Case Summary Review
More than 350 appellate, trial, and supreme court case summaries have been reviewed from different sources.
The sources included NPDB, regional digests, and reports, FindLaw, and MedLaw Internet portals as well as multiple books, newsletters, and journals.
The analysis includes only those cases that meet the following criteria:
- Nurses engaged in the nursing practice as defined by the nurse practice act of their state.
- Nurses that were defendants in civil lawsuits caused by unintentional actions (no criminal cases).
- Trials held 1995 through 2001.
The analysis includes 253 case summaries.
The summaries contain information about the types of negligence, areas of practice, and the outcomes of cases, such as settlements or verdicts of the jury.
Either independent practitioners themselves paid the monetary awards or their employers, on behalf of practitioners.
This is the process occurring according to the doctrine of “respondeat superior” which is Latin for “let the master answer”.
It implies that, in the course of employment, the employer is responsible for the actions of employees.
The majority of reported negligence cases happened in acute care hospitals, which is 60%.
Another 40% took place in long-term care facilities with 18% at rehabilitation and transitional care units and nursing homes, 8% in psychiatric facilities.
Home health agencies and independent practice settings of physicians each were 2%.
The remaining 9% include advanced practice nurses, such as nurse-midwives, nurse practitioners, and nurse anesthetists.
The vast difference between long-term care and acute care facilities lays in the greater number of specialty practice areas in acute care facilities.
Also, it is based on the condition of patients in such areas as EDs, intensive, and obstetrical care, operating and recovery rooms, medical-surgical units, and coronary care.
In these settings, patients may be sicker with quickly changing conditions and require immediate action.
Negligence Issues
Six major categories of negligence issues that lead to malpractice lawsuits were identified in the case review.
The following terms were used in the documentation that described the negligent behavior:
- Lack of.
- Failure to.
- Ineffective.
- Improper.
- Incomplete.
The negligence categories include:
- Failure to use equipment responsibly.
- Failure to follow standards of care.
- Failure to document.
- Failure to communicate.
- Failure to act as a patient advocate.
- Failure to assess and monitor.
Below, you will find summaries of five random cases of malpractice in which nurses became defendants.
They depict a variety of actions that cause breaches in the care standards.

Failure to Follow Standards of Care
Such standards as hospital policies have evolved to ensure that consumers are protected from substandard care.
Standards of care determine the criteria to define if a nurse breached a duty in the care they were to provide to patients.
The acceptable levels of care involve reasonable and ordinary care necessary to ensure that no harm comes to patients.
Standards of care are determined by such bodies as state boards of nursing, guidelines of federal organizations, hospital policies, and procedures.
Such professional nursing associations as ANA or the National League of Nursing can determine the guidelines as well.
Hall v. Arthur case of 1998.
A trial court’s decision upheld by the United States Court of Appeals for the Eighth Circuit under which the hospital was held liable for the nurse breaching the standard of care in an ACF (anterior cervical diskectomy and fusion).
The argument of the plaintiff focused on the use of Orthoblock.
This is a ceramic substance which is used to replace bone in maxillofacial surgery.
It was implanted in the spine of the patient.
In such surgery, the usual procedure would be to either harvest a bone from the patient’s hip or obtain it from a bone bank.
After having complications with his back for four months, the patient, Mr. Hall, needed a second ACF to have his own bone implanted instead of the Orthoblock.
According to the policy of the hospital, any unusual requests to use the product should be reviewed by department managers to determine if the product is appropriate.
The nurse failed to request such a review and ordered the use of Orthoblock in the ACF of the patient.
The product’s package insert was presented as evidence and indicated that Orthoblock was counter-indicative for the spinal procedures.
So the plaintiff’s attorney argument was that the nurse failed to follow the hospital’s policy which resulted in Mr. Hall’s injury.
The hospital didn’t dispute the finding of negligence by the jury but stated that the evidence produced by the plaintiff was insufficient for the judge to conclude that Mr. Hall’s injury resulted from the nurse’s negligence.
The appellate court disagreed, stating that while they couldn’t state certainly that Mr. Hall wouldn’t have been injured if the nurse hadn’t been negligent, they believed that the nurse’s negligence played a significant role allowing the patient to become injured by the Orthoblock.
The assumption was that the surgery wouldn’t have been allowed by the hospital otherwise.
Failure to Use Equipment Responsibly
Nurses should be aware of safety features, limitations, capabilities, and hazards of any equipment they work with.
They should follow the usage recommendations of the manufacturer and keep from modifying it.
Under the Safe Medical Devices Act of 1990, all incidents related to medical devices that can cause serious illness, injury, or death should be reported to the Food and Drug Administration and the manufacturer within 10 working days.
Chin v. St. Barnabas Medical Center case of 1998.
The trial court judgment against the physician was reversed by the Superior Court of New Jersey, Appellate Division.
They defined that other hospital personnel should be held liable.
The case was built on the death of Ms. Chin, a 45-year-old woman.
The death was caused by a massive air embolism in the course of diagnostic hysteroscopy.
The malpractice suit was brought by the woman’s estate against the providers who supposedly played a role in the events that caused her death.
The providers were the physician performing the procedure, one scrub nurse, and two circulating nurses, as well as the hospital, and the manufacturer of the hysteroscope.
The hysteroscope is an optical pump device used to examine the uterus.
In the course of the procedure, fluid is continuously pumped into the uterus to intensify the view of its interior.
The device should be connected to four tubes:
- An irrigation tube flowing fluid into the uterus.
- A suction tube drawing fluid out of the uterus.
- An exhaust tube.
- The tube connecting the compressed nitrogen source to the pump.
One of the tubes was connected to the hysteroscope wrong, and the nitrogen was pumped into the uterus of the patient, which caused a fatal air embolism in her coronary arteries.
At trial, all parties agreed that the source of gas that killed the patient was the exhaust hose.
However, there was a dispute about whose fault was it for attaching the hysteroscope wrong.
According to the presented evidence, the two nurses who were assigned to the procedure didn’t have any experience in the use of a hysteroscope.
They had no hospital training either.
It was revealed that the supervising nurse assigned the providers but wasn’t aware of the lack of experience of other nurses.
The trial wasn’t presented any expert opinion on the standard of care.
At the end of the trial, the members of the jury were instructed by the judge to use their “common knowledge” to decide if the nurses strayed from their duty while caring for Ms. Chin.
The standard of the common-knowledge applies to such facts of the case when the common knowledge and experience of a layperson would allow the juror to conclude if the duty care was breached without the expert’s testimony.
The jury was also informed that Ms. Chin, being unconscious during the procedure, was blameless in her own death.
Also, each defendant had to prove the fault wasn’t theirs.
The plaintiff was awarded $2,000,000 in damages by the jury.
The jury also found the defendants liable by the following percentage:
20% – the physician.
25% – the experienced circulating nurse.
20% – the inexperienced circulating nurse.
35% – the hospital.
The manufacturer and the scrub nurse were cleared of liability.
Right after the verdict, the trial judge governed in favor of the motion of the hospital that questioned whether the applying of the common-knowledge standard in this care was valid.
The judge held only the physician liable.
While granting the hospital’s motions, the judge proclaimed the application of the standard of common-knowledge to be an error.
However, in the appeal of the physician, the appellate court reversed the decision of the trial court and restored the original verdict of the jury.
That meant that each defendant hadn’t established the lack of fault in the death of Ms. Chin entirely.
Also, it was stated that the trial court didn’t fail in the common-knowledge standard application.

Failure to Assess and Monitor and Failure to Communicate
The health status of a patient can change gradually or suddenly.
Nurses are typically the first to notice the changes and act.
The accuracy in monitoring and assessing skills of the nurse as well as their timely report of condition changes to a physician can be a matter between life and death.
Besides the timely report, such aspects as accuracy in communicating the degree and nature of changes and persistence of notifying the physician of them are vital.
Busta v. Columbus Hospital Corporation case of 1996.
The judgment and orders of the District Court of the Eighth Judicial District were affirmed by the Montana Supreme Court.
Mr. Busta was a postoperative patient at Columbus Hospital in Great Falls.
However, he died from injuries that had occurred after he fell from his window on the third floor.
The nurse that was assigned to care for Mr. Busta testified at trial that he had an episode of hypertension and tachycardia during her last visit in the evening.
Besides, he behaved atypically, refused all nursing care and prescribed medication, and desired isolation.
His medication was known to have side effects, including anxiety, confusion, and psychosis.
The nurse failed to report the change in behavior and the symptoms to the physician.
Also, she testified that during her check-up of the patient at midnight, he was sleeping, and she did not reassess the patient’s vital signs.
The patient’s surgeon testified that if he had been notified of the changing symptoms and signs, he would have reassessed Mr. Busta, because of the mind-altering effects of the medication.
According to the expert’s testimony, the nurse was negligent in failing to properly monitor the patient on the night before his death and in failing to report the change of symptoms and signs to the surgeon.
Additionally, it was stated that the hospital was negligent in failing to provide a safe environment.
Based on the evidence presented at trial, it was concluded that the hospital had not followed the JCAHO directive to restrict the windows opening in patients’ rooms.
The jury found that the patient’s injuries and death were the results of the negligence of Columbus Hospital together with contributory negligence of the patient.
70% of liability was appointed to the hospital and 30%, to Mr. Busta, by the jury.
The damage of Mr. Busta’s estate was evaluated in the amount of $5,000, and $800,000, of his heirs.
Based on the liability apportioned by the jury, the court entered a judgment in favor of Mr. Busta’s heirs in the amount of $560,000, and his estate, of $3,500.
Failure to Document
The purpose of documentation is to communicate the information about a patient among providers.
It must accurately reflect the nursing process, including evidence of diagnosis and assessment.
It should include planning for nursing interventions as well as implementation and evaluation of these interventions, and the patient’s response.
Pellerin v. Humedicenters, a case regarding a failure to document nursing procedures.
The trial court’s verdict was affirmed by the Court of Appeals of Louisiana, Fourth Circuit.
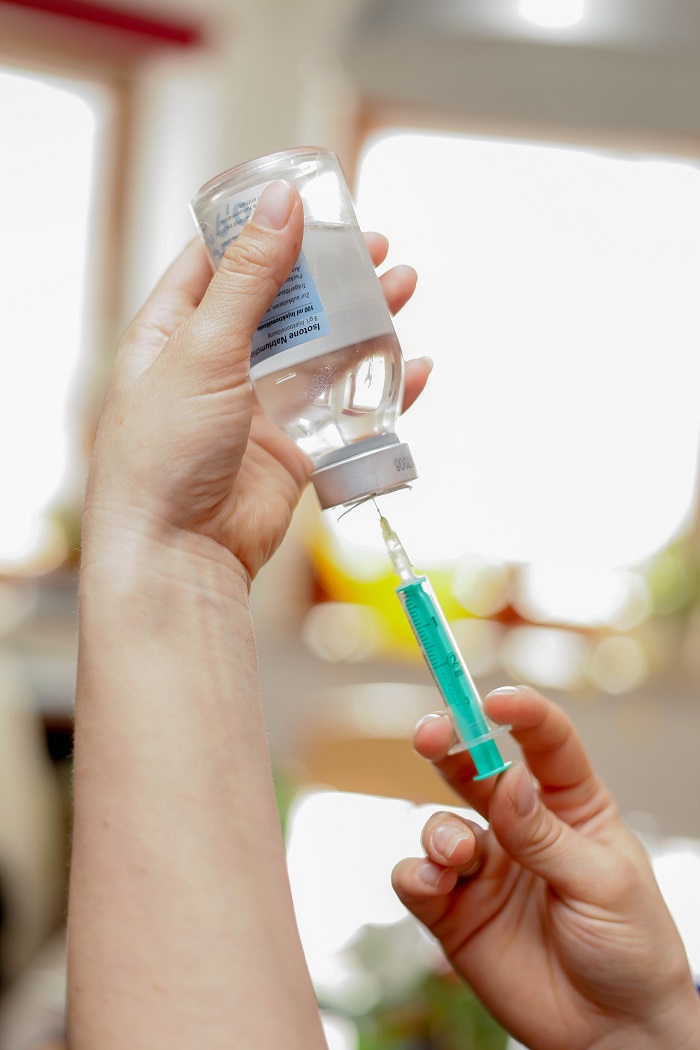
The plaintiff stated that an ED nurse administered an injection of hydroxyzine pamoate (Vistaril) and meperidine (Demerol) in a substandard way.
That caused a lump at the spot of injection and constant pain, which a neurologist later diagnosed as cutaneous gluteal neuropathy.
The trial could not prove how exactly the injury occurred.
The testimony of medical experts concerning the cause of the nerve injury of the patient was conflicting.
It could have been caused by either the needle or the hydroxyzine pamoate.
In the nurse experts’ opinion, the standards of care were neglected by the failure to document the mode and site of injection.
The defendant testified at trial that her regular practice was giving an intramuscular injection and that it met the standards of care.
The jury decided in favor of the plaintiff.
More than $90,000 in damages were awarded.
On appeal, the hospital and the nurse, the defendants, argued that the presented evidence showed that the breach of the standard of care by the nurse couldn’t have caused the injury of the patient.
The appellate court disagreed.
It was stated that the testimony of the nurse, which was insufficient to support the decision of the jury, did not support the decision together with the other evidence at trial.
Failure to Act as a Patient Advocate
Ethical and legal issues can become twisted in the healthcare setting, and nurses should be well-versed in both.
The Code of Ethics for Nurses with Interpretive Statements of ANA provides a guide for decision making related to ethical issues and defines the nurse as a patient advocate.
As stated by O’Keefe in Nursing Malpractice and the Law, in nursing care, patient rights are the advocacy symbol.
Nurses should strive for excellent patient care and the inclusion of their rights in the modern health care system.
Noteworthy, as patient advocates, nurses may have to care for patients whose decisions concerning healthcare may conflict with the ethical beliefs of the nurse.
Koeniquer v. Eckrich case of 1988.
The Circuit Court of the Fifth Judicial Circuit order of summary judgment in favor of Dakota Midland Hospital was remanded and reversed by the Supreme Court of South Dakota.
The case was based on the death of Winnifred Scoblic.
The patient died of sepsis, which was said to have developed when she was discharged about 11 days after urinary tract surgery while having a fever.
The plaintiff, Ms. Koeniquer represented the estate of her mother and initiated a malpractice lawsuit against Dakota Midland Hospital and two physicians.
She claimed that they departed from the appropriate standards of care in postoperative urology.
Ms. Scoblic’s surgery took place on January 5, 1983.
During her postoperative stay, her temperature was varied and, on January 16 at 8:15 am, was recorded at 100.2 F degrees.
It was recorded after her treating physician completed his rounds.
Ms. Scoblic was discharged on the same day at 10:45 am.
On January 19, she was admitted to the hospital again diagnosed with sepsis.
On January 21, the patient was transferred to the University of Minnesota Hospital.
On March 6, she died of multiple organ failure.
The expert witness of the plaintiff stated that nurses failed to properly monitor the changing condition of Ms. Scoblic and provide appropriate postoperative care.
However, they claimed to have reported her elevated temperature and the incision and drainage condition from it to the physician.
They reported it on the day of discharge but such a report wasn’t documented.
The expert also stated that discharging the patient and not providing instructions about monitoring her temperature were cases of failing to act as a patient advocate.
The hospital argued that it was a medical decision to discharge the patient.
However, the director of nursing in the hospital testified that sometimes it’s the responsibility of a nurse to question the order of the physician.
It is especially applicable if the patient’s condition had changed significantly.
The director also confirmed the statement of the expert that it was the nurse’s responsibility to evaluate the patient’s condition independently and pass her concerns to the physician.
If the nurse believed that the decision of the physician had been wrong, she should have had to appeal to other authorities.
The hospital’s argument that a physician decided to discharge the patient was accepted by the court, so the hospital wasn’t an appropriate response to the suit.
However, the state supreme court ruled that the record of the expert’s testimony showed that nurses had the responsibility to attempt to delay the discharge of the patient due to her changing symptoms.
However, the records had no sign of any nurse questioning or disagreeing with the physician’s decision.
The court stated that it was nurses’ duty to question the order of the physician if they thought it would be in the best interest of the patient.
They would have to delay her discharge if they believed it deviated from the appropriate standards of care.
Therefore, the nurse neglected her duty as a patient advocate.
Practice Areas Cited in Complaints

In the course of this review, 13 specialty areas of nurses that were a part of a malpractice suit were identified.
Nurses in the acute care facilities were named defendants who were involved in 153 cases compared to nurses employed in other areas, 100 cases.
Seven specialty practice areas were identified in acute care settings.
The highest percentage (32%) of involvement includes nurses in medical-surgical units, followed by obstetrics units nurses (16%).
Nurses in the following areas in the acute care facilities had the least involvement:
- Operating rooms – 3%.
- Intensive care – 3%.
- Coronary care – 3%.
- Pediatrics – 3%.
- Recovery rooms – 2%.
- ED – 1%.
Outside acute care, six practice areas were identified.
The highest percentage of involvement in litigation included advanced practice nurses working in independent settings (9%).
Next were nurses in psychiatric units, transitional care, and nursing homes (8% each).
The least involved areas included rehabilitation units and home health care units (2% each).
Reducing Potential Liability
The nursing judgment includes the analysis of circumstances and facts based on every case.
For the prevention of malpractice, nurses should initiate this evaluation concerning everything they do in the clinical setting.
More and more often, nurses are held accountable for their judgment and the results it leads to.
Malpractice suits can be emotionally, professionally, and financially disastrous.
Every nurse can take some steps to reduce potential liability by using common sense and caution and maintaining increased awareness of their legal responsibility.
Nurses can do the following to reduce potential liability:
- Keep relations and communication with patients and their family members honest, open, and respectful:
- If patients feel that a nurse was professional and caring, they are less likely to sue.
- Avoid offering opinions if a patient asks what is wrong with them.
You may be blamed for making a diagnosis. - Avoid making statements that can be interpreted as an admission of guilt or fault by a patient.
- When with patients, don’t criticize the actions or health care providers themselves.
- Stay confident in the health care setting.
- Maintain competence in your practice specialty area:
- Increase your knowledge and technical skills.
- Attend relevant hospital in-service and continuing education classes and programs.
- Maintain awareness of legal principles and use them in your daily practice:
- Stay updated with the procedures and policies of the hospital.
- Stay updated with the nurse practice act of your state.
- Keep your practice within the bounds of your license:
- Only perform the skills you are competent in and allowed by your scope of practice.
- Know your strengths and weaknesses.
Don’t accept a clinical assignment you don’t feel competent to perform.- Assess your task with the supervisor.
- Only accept those tasks you are competent to perform.
- For the specialized duties, let an experienced nurse take responsibility.
- Keep accurate records of nursing care.
- If care isn’t recorded, courts will assume it was not provided.
- Use the FACT mnemonic while documenting care on the chart of the patient – factual, accurate, complete, timely.
Six Major Categories of Negligence that Result in Malpractice Lawsuits
Failure to Follow Standards of Care
Including:
- Failure to design a plan of care or complete admission assessment.
- Failure to follow standard institutional policies, procedures, and protocols.
- Failure to follow physicians’ orders, written or verbal.
Failure to Use Equipment Responsibly
Including:
- Failure to follow the recommendations of the manufacturer for operating equipment.
- Failure to check if the equipment is safe before use.
- Failure to place equipment correctly for the treatment.
- Failure to learn the functionality of the equipment.
Failure to Communicate
Including:
- Failure to inform the physician on time when the conditions require it.
- Failure to listen to and take action regarding a patient’s complaints.
- Failure to effectively communicate with a patient.
- Failure to obtain authorization for treatment for higher medical authorities.
Failure to Document
Including failure to include the following in the patient record:
- Response to treatment and progress.
- Injuries.
- Medical orders of a physician.
- Pertinent nursing assessment information.
- Information received via phone conversations with physicians, including the content of the communication, time, and taken actions.

Failure to Assess and Monitor
Including:
- Failure to observe the ongoing progress of the patient.
- Failure to implement a plan of care.
- Failure to interpret symptoms and signs of a patient.
- Failure to complete a shift assessment.
Failure to Act as a Patient Advocate
Including:
- Failure to provide a safe environment.
- Failure to question discharge orders when the condition of the patient requires it.
- Failure to question illegible or incomplete medical orders.
What To Do If You Are Served with a Complaint
Notify your insurance carrier, first of all.
A complaint is a legal application the plaintiff makes to instate a lawsuit.
In includes a statement of the alleged cause or causes of action against the defendant as well as a formal statement.
This can be the first indication of a nurse being named a defendant in a civil lawsuit.
After the complaint is served, the nurse should inform their insurance carrier and employer.
They will usually assign an attorney to the case.
If the nurse doesn’t have liability insurance, they should employ an attorney themselves.
The nurse must discuss the case only with the assigned defense attorney, and no one else.
When notifying the insurance carrier of their liability, the nurse should provide a written description of events.
It should include the place, time, and circumstances of the incident together with the list of addresses and names of the injured party and witnesses.
Once they are served, the nurse should provide all relevant documents to the insurance carrier within the times specified and outlined in the liability insurance policy.
If the nurse fails to notify the insurance carrier within this time, the coverage may be denied.
 by
by